Desk job? Low back pain in the office? Here’s why your hip flexors could be the culprit.
If you work a desk job and experience persistent low back pain, your daily sitting habits may be the underlying cause.
Many professionals commuting into the CBD from Hawthorn spend anywhere from 6 to 10 hours per day seated. While this feels normal in today’s society, humans were not designed for prolonged static sitting. We’re built for variability: walking, rotating, loading, extending, hinging. When you hold the body in hip flexion for 6–10 hours a day, predictable adaptations occur.
Let’s break down what’s actually happening.
From a biomechanical standpoint, sustained sitting places the hips into approximately 90° of flexion. When this becomes the dominant daily posture:
Hip flexors adaptively shorten
Gluteal activity decreases
Lumbar segments experience prolonged flexion or compensatory extension
Deep stabilisers reduce activation
The issue isn’t sitting occasionally.
It’s chronic exposure without counterbalance.
Tight Hip Flexors and Anterior Pelvic Tilt
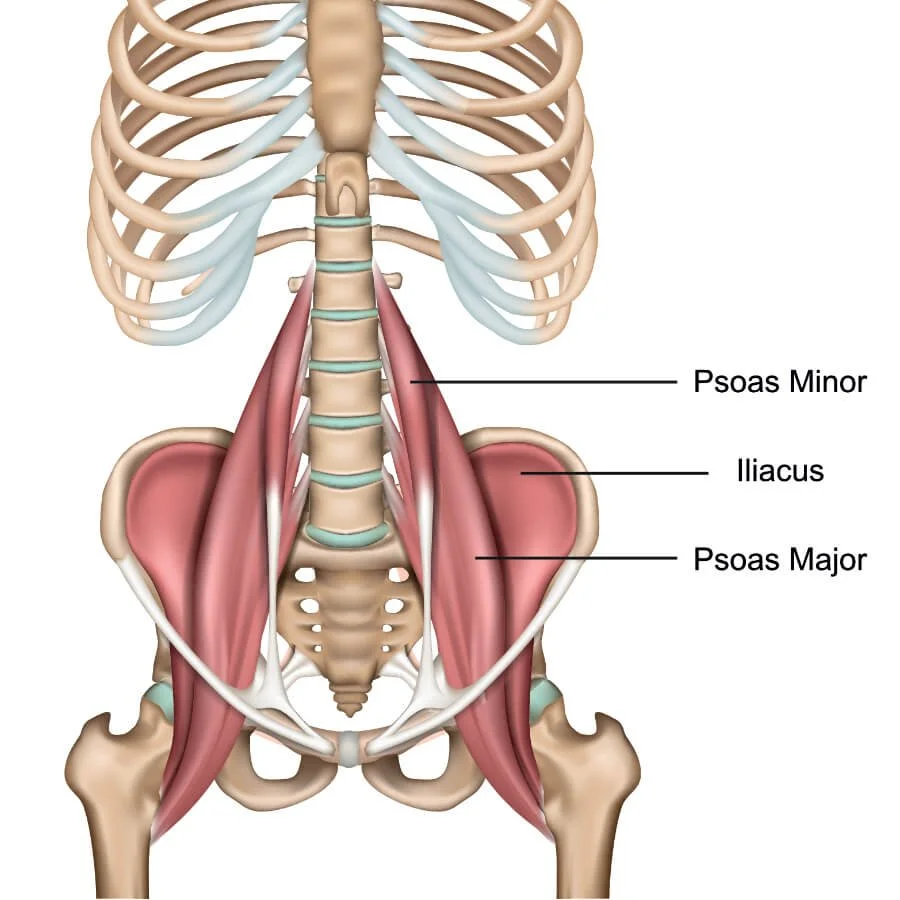
The primary hip flexor complex
The iliopsoas — originates from the lumbar vertebrae and inserts onto the femur.
The iliacus - originated from the iliac crest (hip bone) and inserts onto the femur
When shortened over time, these two muscles can:
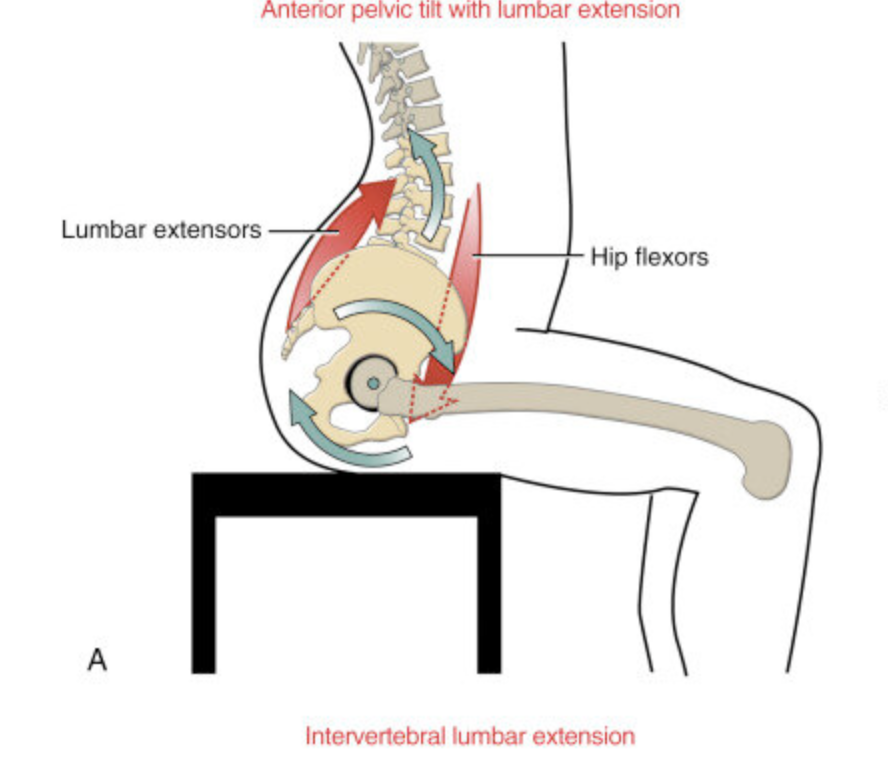
Increase anterior pelvic tilt
Increase lumbar lordosis
Increase compressive load on posterior spinal elements
Anterior pelvic tilt shifts the pelvis forward, the lower spine extends excessively. This increases compressive stress on the posterior elements of the lumbar spine — a common driver of mechanical low back pain.
This can lead to:
Compression of lumbar facet joints
Recurrent lower back stiffness
Lumbar Facet Joint Compression
The lumbar facet joints are small articulations at the back of each vertebral segment. Their role is to guide and control movement.
When lumbar extension becomes excessive (often secondary to anterior pelvic tilt), these joints experience:
Increased compressive forces
Local inflammation
Mechanical irritation
Recurrent “stiff” or “pinching” sensations
Many people interpret this as “my back is tight.”
In reality, it’s often joint compression driven by pelvic positioning.
Glute and Core Disengagement
Prolonged sitting also impacts muscular activation patterns.
When seated:
The gluteus maximus is in a lengthened, inactive position
The abdominal wall becomes passive
Intra-abdominal pressure regulation decreases
Over time, this reduces the body’s ability to stabilise the pelvis dynamically.
When you then stand up and go straight into training — squats, deadlifts, running — the stabilising system is underprepared.
This mismatch between passive posture and high load demand is where flare-ups occur.
The Multifidus: The Overlooked Stabiliser
One of the most important but under-discussed muscles in lumbar stability is the multifidus.
The multifidus:
Attaches segmentally between vertebrae
Provides fine motor control and segmental stabilisation
Prevents excessive micro-movement at each spinal level
Research shows that prolonged low-level inactivity (like sustained sitting) can reduce multifidus activation and even lead to atrophy in cases of persistent low back pain.
When the multifidus underperforms:
Segmental control decreases
Shear forces increase
Facet compression may worsen
Pain becomes recurrent rather than acute
In simple terms:
Your spine loses its local stabilising control.
Why Stretching Alone Isn’t Enough
Yes — hip flexor mobility work is important.
But long-term resolution requires:
Pelvic position control
Glute strength restoration
Core reactivation
Graded spinal loading
Endurance training of deep stabilisers (including multifidus)
Mobility without motor control doesn’t change mechanics.
Strength without control reinforces compensation.
The key is integration.
Practical Takeaways for Desk Workers
If you commute into the city and sit most of the day:
Break up sitting every 45–60 minutes
Perform hip extension work daily
Include glute activation before training
Train anti-extension core stability
Don’t ignore recurrent stiffness
When To Seek Assessment
You should consider a professional assessment if you have:
Low back pain lasting more than two weeks
Recurrent flare-ups
Pain radiating into the glutes or leg
Reduced strength or performance in training
Addressing the root cause early prevents chronic patterns from developing.
Final Thought
Low back pain in desk-based professionals is rarely about “a weak back.”
It’s usually about:
Sustained hip flexion
Anterior pelvic positioning
Lumbar facet compression
Glute inhibition
Multifidus underactivation